|
by Ben Williams '16  "Sometimes it's said that psychiatrists "Sometimes it's said that psychiatristsare doctors who are frightened by the sight of blood. I might have fallen into that category." [image via] When asked how he remains sane while studying the psychological effects of harrowing experiences, renowned psychiatrist and author Robert J. Lifton replies, "I draw bird cartoons." "We need a sense of absurdity, sometimes gallows humor, to survive the absurdities of our world," said Dr. Lifton in a speech entitled "Research as Witness: A Psychiatrist’s Struggles with Extreme Events," delivered at Brown on October 21, 2013 as the 21st annual Harriet W. Sheridan Literature and Medicine Lecture. The 87-year-old Brooklyn native has held positions at Harvard, Yale, and the John Jay College of Criminal Justice. He has published over 20 books on the psychological consequences of historical events. Over the course of his career, Lifton has interviewed American prisoners of war, survivors of Hiroshima, and Nazi doctors. After two years in the Air Force in Korea and Japan, Lifton embarked on the "struggle to bring together psychology and history." Eschewing the ideally objective approach of scientific research, Dr. Lifton found himself constantly motivated by ethical concerns and a desire to participate in what he calls "relevant activism."
0 Comments
by Nari Lee '17  Sex differences can create problems both in pain and its treatment. This topic adds yet another aspect to today’s complex sex/gender equality debate, but it’s highly relevant for anyone who experiences pain – namely, everyone. Research has revealed that males and females perceive pain differently, yet management of pain for men and women doesn't take that into account. In fact, treatment of pain is often generalized for both sexes (or worse, biased). Instead, doctors should tailor treatments to the differences in female and male bodies’ responses to pain and pain medicine. To do this, though, greater research is needed on sex-specific responses to pain treatments. by Denise Croote '16 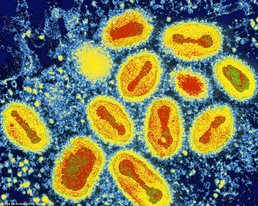 Not your mama's SpaghettiOs. [image via] Not your mama's SpaghettiOs. [image via] It seems as though the Mayans made a slight miscalculation. In 2012 we narrowly escaped a meteor storm and a black hole to live another day, but we’re definitely not free from danger. Certain dangers we can see and fear, like tornadoes and sandstorms, but other hazards are far less evident. Viruses are very good at slipping under our radar, mainly because we can’t see them, and only become aware of their presence when they infect our population. Smallpox, an infectious disease responsible for an estimated 300 to 500 million deaths in the 20th century, might just be back to haunt us (1). When the WHO organization announced the universal eradication of smallpox in 1980, smallpox vaccinations were discontinued in the United States and several other industrialized countries. By 1985, routine vaccinations were eliminated across the globe. This act reduced health care costs, but left us with a population susceptible to a smallpox outbreak (1). If the smallpox virus were to fall into the wrong hands, it would be a deadly bio-terror weapon. Our vulnerable population would guarantee the rapid propagation of the disease and to this date there is no known cure. Smallpox begins with a simple fever and quickly proceeds to a systemic rash. The rash develops into firm pustules that eventually crust over and scar. Approximately 30% of those who are infected with smallpox die from the disease. This would undoubtedly result in mass sickness and widespread panic if ever released in the United States (2). by Denise Croote '16 Believe it or not, cannibalism isn’t a thing of the distant past. As recent as the 1950s, villagers on the island of New Guinea actively practiced cannibalism. After the death of a loved one, relatives gathered to bless and consume the body. The women and children led the ceremony, while the males refrained from partaking in the feast. Interestingly, the women and children started to develop an unrecognized neurological disorder, while the males did not. Kuru, as they called it, was a disorder in which the infected individual shook, failed to complete simple motor commands, and refused nourishment. The natives claimed the spirits sent Kuru to them as a punishment, but Michael Alpers, an Australian medical researcher, wasn’t convinced. Dedicating his entire life to investigating Kuru, Alpers made a shocking discovery that turned our understanding of diseases upside down. Could a neurological disorder really be contagious? And could cannibalism fuel its transmission? To learn more about Alpers and his work, watch the documentary Kuru: The Science and the Sorcery below, or check out the article "The Last Laughing Death" at The Global Mail. by Jennifer Maccani, PhD This is part 3 of a 3-part article. This article is part of the "Emerging Biotechnology" series. It all began in 2008. That was the year Organovo Holdings, Inc. founder Dr. Gabor Forgacs of the University of Missouri–Columbia published an article in the journal Tissue Engineering Part A describing the first ever bioprinted blood vessel construct from chicken cells (15, 16). Rather than growing cells in a flat layer covered by cell culture media with the nutrients necessary for the cells’ survival, Dr. Forgacs and his colleagues had printed cells, or “bio-ink,” and collagen scaffolding (“bio-paper”) into a living three-dimensional structure (15). The beauty of his approach was that in a three-dimensional environment, the cells were free to do what their DNA programmed them to do—fuse with their neighbors and behave as they would in the body. This process of “self-assembly,” Dr. Forgacs explains, allows cells to retain their natural shape and characteristics that can sometimes be lost in the context of traditional two-dimensional cell culturing, such as in a petri dish (15). In the case of the chicken blood vessel constructs, the cells began to contract and “beat” (15)—just like a heart (16). If you’re still imagining the plight of the patient with heart failure, that’s good news—very good news. And it gets better.
by Jennifer Maccani, PhD This is part 2 of a 3-part article. This article is part of the "Emerging Biotechnology" series. A network of 3D printers is already beginning to form at Brown. One 3D printer is already in use in the laboratory of Dr. Kenneth Breuer, a fluid mechanist, and Dr. Sharon Swartz, a biologist focused on morphology and functional biology. Cosima Schunk, a graduate student in the lab, is a PhD candidate in the School of Engineering’s Biomedical Engineering Program just entering her fourth year. “My research is inspired by biomimetics, that’s my undergrad degree, and I’m looking at bat flight and possible application towards the development of engineering devices like micro-air vehicles,” Schunk says. One can tell from her undergraduate education at the University of Applied Sciences in Bremen, Germany, that Schunk is serious about the research of biomimetics; as she says, “It was the first school in Germany, actually, where you could directly study biomimetics.” As Schunk describes it, biomimetics is “generally learning from nature and applying biological concepts to engineering.” Although Schunk studies bats, “the idea, generally, is you look at bio-solutions evolved by nature and then you see if you can abstract the concept, and then apply this abstract concept towards an engineering solution.”  A bird emitting brightly colored chain links of goo. Or a model of how a bird's flapping wings create aerodynamic effects. [image via] In a recent publication in the Journal of Bioinspiration and Biomimetics (11), a former graduate student named Joseph Bahlman with whom Cosima Schunk has worked, together with Drs. Breuer and Swartz, characterized the robotic bat wing, or “flapper” as Schunk refers to it, that they designed and 3D-printed to study bat flight. “[Bats] are really agile flyers, very maneuverable, but we don’t know a lot about how they are actually doing it,” Schunk explains. “There’s a lot of engineering work out there looking at aeromechanical, aerodynamical behavior of membranous wings.”
by Jennifer Maccani, PhD This is part 1 of a 3-part article. This article is part of the "Emerging Biotechnology" series. Imagine being a patient with heart failure, waiting on the heart transplant list, knowing that a new heart is the only chance for your survival. Although you know that gaining your new life rests on someone else’s loss, you can’t help but hope that you might somehow be able to get to the top of the transplant list in time. Even if you do, there’s no guarantee that your body won’t reject the new heart, or that you’ll be able to tolerate potentially dangerous immunosuppressive drugs. Nearly 25% of heart transplant recipients suffer from organ rejection in the first year after transplantation (1). Now imagine that rather than waiting on the transplant list, your doctor could grow you a new heart and transplant it—without the harsh side effects of immunosuppressive drugs (2)—from your very own cells. That scenario may soon be a reality, thanks to a new technology called three-dimensional (3D) bioprinting. 3D bioprinting works like other types of 3D printing. Rather than depositing ink, 3D printers dispense materials such as plastic in consecutive layers according to a digital model to produce a three-dimensional structure (3). In this same vein, 3D bioprinters dispense spheres of cells—even, hopefully, a patient’s own cells—into a gel mold or scaffold to produce an organ or tissue (4). With bioprinting technology, tissues could potentially be used for transplants or for research. Furthermore, bioprinting has initiated a paradigm shift that could reduce the current reliance on animal models in studies of human diseases and in preclinical pharmaceutical drug testing (4). |
